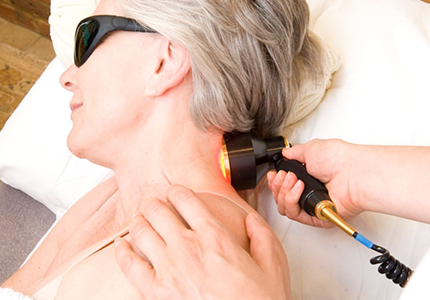
Figure 7. Application of red/near-infrared LLLT and LED to treat neck pain.
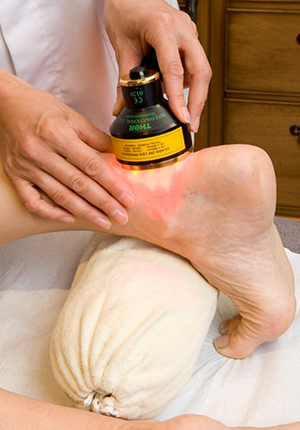
Figure 8. Application of red/near-infrared LLLT and LED to treat the Achilles tendon.
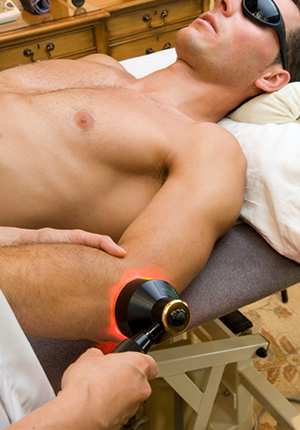
Figure 9. Application of red/near-infrared LLLT and LED to treat the elbow (lateral epicondylitis).
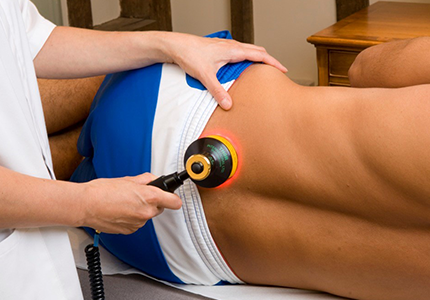
Figure 10. Application of red/near-infrared LLLT and LED to treat low back pain.
Musculoskeletal Dysfunction and Pain
Musculoskeletal pain and dysfunction is the leading cause of disability and far exceeds the cost of all other healthcare categories, including diabetes, heart disease, cancer, and all forms of dementia.
The positive effects of photobiomodulation (PBM) therapy on musculoskeletal pain and dysfunction (by low-level laser or LED) has been reported in over 120 randomized controlled clinical trials (RCTs). These include back pain, neck pain, tendinopathies (tennis elbow, shoulder tendinopathies, achilles tendinopathies), osteoarthritis, rheumatoid arthritis, ankle sprains, myofascial pain, TMJ pain, carpal tunnel syndrome, repetitive strain injuries and other soft tissue injuries, etc.
A Pubmed search for “pain” and PBM (and a range of alternative terms such as LLLT and laser biostimulation) returns 985 results. The effect of PBM therapy on pain has been explored more than any other clinical category and is by far the most common clinical application in medical practice today.
Many systematic reviews have been performed with the following conclusions.
Chow et al., 2009, The Lancet: “LLLT reduces pain immediately after treatment in acute neck pain and up to 22 weeks after completion of treatment in patients with chronic neck pain”[1]. 19913903
Glazed et al., 2016, Acupunct Med BMJ: “We demonstrated moderate quality of evidence to support a clinically important benefit in LLLT for chronic non-specific low back pain in the short term” [2]
Bjordal et al., 2003, Australian Journal Physiotherapy: “Low level laser therapy with the suggested dose range significantly reduces pain and improves health status in chronic joint disorders” [3]
Tumilty et al., 2009, Photomedicine and laser surgery: “LLLT can potentially be effective in treating tendinopathy when recommended dosages are used. The 12 positive studies provide strong evidence that positive outcomes are associated with the use of current dosage recommendations for the treatment of tendinopathy”[4]
Figures 7, 8, 9 and 10 show application of red/near-infrared low-level laser therapy (LLLT) or LED to treat pain in musculoskeletal injures (acute or chronic).
1. Chow, R.T., et al., Efficacy of low-level laser therapy in the management of neck pain: a systematic review and meta-analysis of randomised placebo or active-treatment controlled trials. Lancet, 2009. 374(9705): p. 1897-908.
2. Glazov, G., M. Yelland, and J. Emery, Low-level laser therapy for chronic non-specific low back pain: a meta-analysis of randomised controlled trials. Acupunct Med, 2016.
3. Bjordal, J.M., et al., A systematic review of low level laser therapy with location-specific doses for pain from chronic joint disorders. Aust J Physiother, 2003. 49(2): p. 107-16.
4. Tumilty, S., et al., Low level laser treatment of tendinopathy: a systematic review with meta-analysis. Photomed Laser Surg, 2010. 28(1): p. 3-16.
5. Naeser MA. Photobiomodulation of Pain in Carpal Tunnel Syndrome: Review of Seven Laser Therapy Studies. Photomedicine and Laser Surgery, 2006. 24(2): p. 101-110.
Video Link